NEET MDS Lessons
Orthodontics
Expansion in orthodontics refers to the process of widening the dental arch to create more space for teeth, improve occlusion, and enhance facial aesthetics. This procedure is particularly useful in treating dental crowding, crossbites, and other malocclusions. The expansion can be achieved through various appliances and techniques, and it can target either the maxillary (upper) or mandibular (lower) arch.
Types of Expansion
-
Maxillary Expansion:
- Rapid Palatal Expansion (RPE):
- Description: A common method used to widen the upper jaw quickly. It typically involves a fixed appliance that is cemented to the molars and has a screw mechanism in the middle.
- Mechanism: The patient or orthodontist turns the screw daily, applying pressure to the palatine suture, which separates the two halves of the maxilla, allowing for expansion.
- Indications: Used for treating crossbites, creating space for crowded teeth, and improving the overall arch form.
- Duration: The active expansion phase usually lasts about 2-4 weeks, followed by a retention phase to stabilize the new position.
- Rapid Palatal Expansion (RPE):
-
Slow Palatal Expansion:
- Description: Similar to RPE but involves slower, more gradual expansion.
- Mechanism: A fixed appliance is used, but the screw is activated less frequently (e.g., once a week).
- Indications: Suitable for patients with less severe crowding or those who may not tolerate rapid expansion.
-
Mandibular Expansion:
- Description: Less common than maxillary expansion, but it can be achieved using specific appliances.
- Mechanism: Appliances such as the mandibular expansion appliance can be used to widen the lower arch.
- Indications: Used in cases of dental crowding or to correct certain types of crossbites.
Mechanisms of Expansion
- Skeletal Expansion: Involves the actual widening of the bone structure (e.g., the maxilla) through the separation of the midpalatine suture. This is more common in growing patients, as their bones are more malleable.
- Dental Expansion: Involves the movement of teeth within the alveolar bone. This can be achieved through the application of forces that move the teeth laterally.
Indications for Expansion
- Crossbites: To correct a situation where the upper teeth bite inside the lower teeth.
- Crowding: To create additional space for teeth that are misaligned or crowded.
- Improving Arch Form: To enhance the overall shape and aesthetics of the dental arch.
- Facial Aesthetics: To improve the balance and symmetry of the face, particularly in growing patients.
Advantages of Expansion
- Increased Space: Creates additional space for teeth, reducing crowding and improving alignment.
- Improved Function: Corrects functional issues related to occlusion, such as crossbites, which can lead to better chewing and speaking.
- Enhanced Aesthetics: Improves the overall appearance of the smile and facial profile.
- Facilitates Orthodontic Treatment: Provides a better foundation for subsequent orthodontic procedures.
Limitations and Considerations
- Age Factor: Expansion is generally more effective in growing children and adolescents due to the flexibility of their bones. In adults, expansion may require surgical intervention (surgical-assisted rapid palatal expansion) due to the fusion of the midpalatine suture.
- Discomfort: Patients may experience discomfort or pressure during the expansion process, especially with rapid expansion.
- Retention: After expansion, a retention phase is necessary to stabilize the new arch width and prevent relapse.
- Potential for Relapse: Without proper retention, there is a risk that the teeth may shift back to their original positions.
Growth is the increase in size It may also be defined as the normal� change in the amount of living substance. eg. Growth is the quantitative aspect and measures in units of increase per unit of time.
Development
It is the progress towards maturity (Todd). Development may be defined as natural sequential series of events between fertilization of ovum and adult stage.
Maturation
It is a period of stabilization brought by growth and development.
CEPHALOCAUDAL GRADIENT OF GROWTH
This simply means that there is an axis of increased growth extending from the head towards feet. At about 3rd month of intrauterine life the head takes up about 50% of total body length. At this stage cranium is larger relative to face. In contrast the limbs are underdeveloped.�
By the time of birth limbs and trunk have grown faster than head and the entire proportion of the body to the head has increased. These processes of growth continue till adult.��
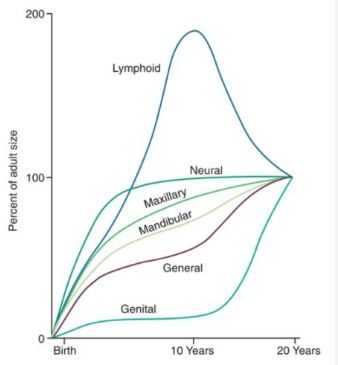
SCAMMON�S CURVE
In normal growth pattern all the tissue system of the body do not growth at the same rate. Scammon�s curve for growth shows 4 major tissue system of the body;
� Neural
� Lymphoid�
� General: Bone, viscera, muscle.
� Genital
The graph indicates the growth of the neural tissue is complete by 6-7 year of age. General body tissue show an �S� shaped curve with showing of rate during childhood and acceleration at puberty. Lymphoid tissues proliferate to its maximum in late childhood and undergo involution. At the same time growth of the genital tissue accelerate rapidly.�
�
SEQUENCE OF ERUPTION OF DECIDUOUS TEETH
Upper/Lower A B D C E
SEQUENCE OF ERUPTION OF PERMAMENT TEETH
Upper: 6 1 2 4 3 5 7 Lower: 6 1 2 3 4 5 7
or 6 1 2 4 5 3 7 or 6 1 2 4 3 5 7
ANTHROPOID SPACE / PRIMATE SPACE / SIMIEN’S SPACE
The space mesial to upper deciduous canine and distal to lower deciduous canine is characteristically found in primates and hence it is called primate space.
INCISOR LIABILITY
When the permanent central incisor erupt, these teeth use up specially all the spaces found in the normal dentition. With the eruption of permanent lateral incisor the space situation becomes tight. In the maxillary arch it is just enough to accommodate but in mandibular arch there is an average 1.6 mm less space available. This difference between the space present and space required is known as incisor liability.
These conditions overcome by;
1. This is a transient condition and extra space comes from slight increase in arch width.
2. Slight labial positioning of central and lateral incisor.
3. Distal shift of permanent canine.
LEE WAY SPACE (OF NANCE)
The combined mesiodistal width of the permanent canines and pre molars is usually less that of the deciduous canines and molars. This space is
called leeway space of Nance.
Measurement of lee way space:
Is greater in the mandibular arch than in the maxillary arch It is about 1.8mm [0.9mm on each side of the arch] in the maxillary arch.
And about 3.4mm [1.7 mm on side of the arch] in the mandibular arch.
Importance:
This lee way space allows the mesial movement of lower molar there by correcting flush terminal plane.
LWS can be measure with the help of cephalometry.
FLUSH TERMINAL PLANE (TERMINAL PLANE RELATIONSHIP)
Mandibular 2nd deciduous molar is usually wider mesio-distally then the maxillary 2nd deciduous molar. This leads to the development of flush terminal plane which falls along the distal surface of upper and lower 2nd deciduous molar. This develops into class I molar relationship.
Distal step relationship leads to class 2 relationship.
Mesial step relationship mostly leads to class 3 relationship.
FEATURE OF IDEAL OCCLUSION IN PRIMARY DENTITION
1. Spacing of anterior teeth.
2. Primate space is present.
3. Flush terminal plane is found.
4. Almost vertical inclination of anterior teeth.
5. Overbite and overjet varies.
UGLY DUCKLING STAGE
Definition:
Stage of a transient or self correcting malocclusion is seen sometimes is called ugly duck ling stage.
Occurring site: Maxillary incisor region
Occuring age: 8-9 years of age.
This situation is seen during the eruption of the permanent canines. As the developing p.c. they displace the roots of lateral incisor mesially this results is transmitting of the force on to the roots of the central incisors which also gets displaced mesially. A resultant distal divergence of the crowns of the two central incisors causes midline spacing.
This portion of teeth at this stage is compared to that of ugly walk of the duckling and hence it is called Ugly Duckling Stage.
Described by Broad bent. In this stage children tend to look ugly. Parents are often apprehensive during this stage and consult the dentist.
Corrects by itself, when canines erupt and the pressure is transferred from the roots to the coronal area of the incisor.
IMPORTANCE OF 1ST MOLAR
1. It is the key tooth to occlusion.
2. Angle’s classification is based on this tooth.
3. It is the tooth of choice for anchorage.
4. Supports occlusion in a vertical direction.
5. Loss of this tooth leads to migration of other tooth.
6. Helps in opening the bite.
Relapse
Definition: Relapse refers to the tendency of teeth to return to their original positions after orthodontic treatment. This can occur due to various factors, including the natural elasticity of the periodontal ligament, muscle forces, and the influence of oral habits.
Causes of Relapse
- Elasticity of the Periodontal Ligament: After orthodontic treatment, the periodontal ligament may still have a tendency to revert to its original state, leading to tooth movement.
- Muscle Forces: The forces exerted by the lips, cheeks, and tongue can influence tooth positions, especially if these forces are not balanced.
- Growth and Development: In growing patients, changes in jaw size and shape can lead to shifts in tooth positions.
- Non-Compliance with Retainers: Failure to wear retainers as prescribed can significantly increase the risk of relapse.
Prevention of Relapse
- Consistent Retainer Use: Adhering to the retainer regimen as prescribed by the orthodontist is crucial for maintaining tooth positions.
- Regular Follow-Up Visits: Periodic check-ups with the orthodontist can help monitor tooth positions and address any concerns early.
- Patient Education: Educating patients about the importance of retention and the potential for relapse can improve compliance with retainer wear.
Angle�s Classification of Malocclusion
Malocclusion refers to the misalignment or incorrect relationship between the teeth of the two dental arches when they come into contact as the jaws close. Understanding occlusion is essential for diagnosing and treating orthodontic issues.
Definitions
- Occlusion: The contact between the teeth in the mandibular arch and those in the maxillary arch during functional relations (Wheeler�s definition).
- Malocclusion: A condition characterized by a deflection from the normal relation of the teeth to other teeth in the same arch and/or to teeth in the opposing arch (Gardiner, White & Leighton).
Importance of Classification
Classifying malocclusion serves several purposes:
- Grouping of Orthodontic Problems: Helps in identifying and categorizing various orthodontic issues.
- Location of Problems: Aids in pinpointing specific areas that require treatment.
- Diagnosis and Treatment Planning: Facilitates the development of effective treatment strategies.
- Self-Communication: Provides a standardized language for orthodontists to discuss cases.
- Documentation: Useful for recording and tracking orthodontic problems.
- Epidemiological Studies: Assists in research and studies related to malocclusion prevalence.
- Assessment of Treatment Effects: Evaluates the effectiveness of orthodontic appliances.
Normal Occlusion
Molar Relationship
According to Angle, normal occlusion is defined by the relationship of the mesiobuccal cusp of the maxillary first molar aligning with the buccal groove of the mandibular first molar.
Angle�s Classification of Malocclusion
Edward Angle, known as the father of modern orthodontics, first published his classification in 1899. The classification is based on the relationship of the mesiobuccal cusp of the maxillary first molar to the buccal groove of the mandibular first molar. It is divided into three classes:
Class I Malocclusion (Neutrocclusion)
- Definition: Normal molar relationship is present, but there may be crowding, misalignment, rotations, cross-bites, and other irregularities.
- Characteristics:
- Molar relationship is normal.
- Teeth may be crowded or rotated.
- Other alignment irregularities may be present.
Class II Malocclusion (Distocclusion)
- Definition: The lower molar is positioned distal to the upper molar.
- Characteristics:
- Often results in a retrognathic facial profile.
- Increased overjet and overbite.
- The mesiobuccal cusp of the maxillary first molar occludes anterior to the buccal groove of the mandibular first molar.
Subdivisions of Class II Malocclusion:
- Class II Division 1:
- Class II molars with normally inclined or proclined maxillary central incisors.
- Class II Division 2:
- Class II molars with retroclined maxillary central incisors.
Class III Malocclusion (Mesiocclusion)
- Definition: The lower molar is positioned mesial to the upper molar.
- Characteristics:
- Often results in a prognathic facial profile.
- Anterior crossbite and negative overjet (underbite).
- The mesiobuccal cusp of the upper first molar falls posterior to the buccal groove of the lower first molar.
Advantages of Angle�s Classification
- Comprehensive: It is the first comprehensive classification and is widely accepted in the field of orthodontics.
- Simplicity: The classification is straightforward and easy to use.
- Popularity: It is the most popular classification system among orthodontists.
- Effective Communication: Facilitates clear communication regarding malocclusion.
Disadvantages of Angle�s Classification
- Limited Plane Consideration: It primarily considers malocclusion in the anteroposterior plane, neglecting transverse and vertical dimensions.
- Fixed Reference Point: The first molar is considered a fixed point, which may not be applicable in all cases.
- Not Applicable for Deciduous Dentition: The classification does not effectively address malocclusion in children with primary teeth.
- Lack of Distinction: It does not differentiate between skeletal and dental malocclusion.
Nail Biting Habits
Nail biting, also known as onychophagia, is one of the most common habits observed in children and can persist into adulthood. It is often associated with internal tension, anxiety, or stress. Understanding the etiology, clinical features, and management strategies for nail biting is essential for addressing this habit effectively.
Etiology
-
Emotional Problems:
- Persistent nail biting may indicate underlying emotional issues, such as anxiety, stress, or tension. It can serve as a coping mechanism for dealing with these feelings.
-
Psychosomatic Factors:
- Nail biting can be a psychosomatic response to stress or emotional discomfort, manifesting physically as a way to relieve tension.
-
Successor of Thumb Sucking:
- For some children, nail biting may develop as a successor to thumb sucking, particularly as they transition from one habit to another.
Clinical Features
-
Dental Effects:
- Crowding: Nail biting can contribute to dental crowding, particularly if the habit leads to changes in the position of the teeth.
- Rotation: Teeth may become rotated or misaligned due to the pressure exerted during nail biting.
- Alteration of Incisal Edges: The incisal edges of the anterior teeth may become worn down or altered due to repeated contact with the nails.
-
Soft Tissue Changes:
- Inflammation of Nail Bed: Chronic nail biting can lead to inflammation and infection of the nail bed, resulting in redness, swelling, and discomfort.
Management
-
Awareness:
- The first step in management is to make the patient aware of their nail biting habit. Understanding the habit's impact on their health and appearance can motivate change.
-
Addressing Emotional Factors:
- It is important to identify and treat any underlying emotional issues contributing to the habit. This may involve counseling or therapy to help the individual cope with stress and anxiety.
-
Encouraging Outdoor Activities:
- Engaging in outdoor activities and physical exercise can help reduce tension and provide a positive outlet for stress, potentially decreasing the urge to bite nails.
-
Behavioral Modifications:
- Nail Polish: Applying a bitter-tasting nail polish can deter nail biting by making the nails unpalatable.
- Light Cotton Mittens: Wearing mittens or gloves can serve as a physical reminder to avoid nail biting and can help break the habit.
-
Positive Reinforcement:
- Encouraging and rewarding the individual for not biting their nails can help reinforce positive behavior and motivate them to stop.
Springs in Orthodontics
Springs are essential components of removable orthodontic appliances, playing a crucial role in facilitating tooth movement. Understanding the mechanics of springs, their classifications, and their applications is vital for effective orthodontic treatment.
- Springs are active components of removable orthodontic appliances that deliver forces to teeth and/or skeletal structures, inducing changes in their positions.
- Mechanics of Tooth Movement: To achieve effective tooth movement, it is essential to apply light and continuous forces. Heavy forces can lead to damage to the periodontium, root resorption, and other complications.
Components of a Removable Appliance
A removable orthodontic appliance typically consists of three main components:
- Baseplate: The foundation that holds the appliance together and provides stability.
- Active Components: These include springs, clasps, and other elements that exert forces on the teeth.
- Retention Components: These ensure that the appliance remains in place during treatment.
Springs as Active Components
Springs are integral to the active components of removable appliances. They are designed to exert specific forces on the teeth to achieve desired movements.
Components of a Spring
- Wire Material: Springs are typically made from stainless steel or other resilient materials that can withstand repeated deformation.
- Shape and Design: The design of the spring influences its force delivery and stability.
Classification of Springs
Springs can be classified based on various criteria:
1. Based on the Presence or Absence of Helix
- Simple Springs: These springs do not have a helix and are typically used for straightforward tooth movements.
- Compound Springs: These springs incorporate a helix, allowing for more complex movements and force applications.
2. Based on the Presence of Loop or Helix
- Helical Springs: These springs feature a helical design, which provides a continuous force over a range of motion.
- Looped Springs: These springs have a looped design, which can be used for specific tooth movements and adjustments.
3. Based on the Nature of Stability
- Self-Supported Springs: Made from thicker gauge wire, these springs can support themselves and maintain their shape during use.
- Supported Springs: Constructed from thinner gauge wire, these springs lack adequate stability and are often encased in a metallic tube to provide additional support.
Applications of Springs in Orthodontics
- Space Maintenance: Springs can be used to maintain space in the dental arch during the eruption of permanent teeth.
- Tooth Movement: Springs are employed to move teeth into desired positions, such as correcting crowding or aligning teeth.
- Retention: Springs can also be used in retainers to maintain the position of teeth after orthodontic treatment.
